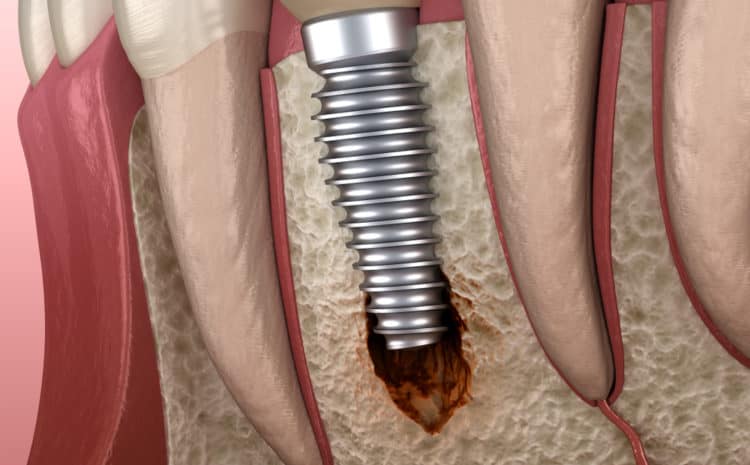
The Silent Threat: Understanding Peri-Implantitis
Peri-implantitis is a disorder that affects people who have had dental implants. It all begins with bacteria forming in the gums around the implant. It's similar to gum disease in that it damages the gums and teeth around it in numerous ways. Getting dental implants, on the other hand, does not guarantee that you will develop peri-implantitis. If found early enough, it is easily avoided and cured.
What is peri implantitis?
Peri-implantitis is a dental condition in which the soft and hard gum tissues around a dental implant become inflamed. Peri-implantitis is identified by bone loss around the inflammatory gums that support the tooth implant.
What are the risk factors of peri-implantitis?
Peri-implantitis is a condition that can affect patients who have implants. The gums around a tooth implant become inflected, causing peri-implantitis. The following are some of the causes and risk factors for peri-implantitis:
- Oral hygiene issues
- Tobacco consumption
- Systemic diseases that aren’t well-controlled (e.g., diabetes mellitus, osteoporosis)
- Periodontal disease incidence and treatment non-adherence
- Other parafunctional habits such as bruxism (grinding teeth)
- Premature loading and poor implant stability throughout the healing phase
How to diagnose peri-implantitis?
When your dentist takes an X-ray of your tooth or jawbone, you can see that the bone that supports the implant will appear to be receding. Your dentist can observe changes in your gum color, bleeding, increased probing depth of gingival pockets around your implant, and suppuration.
What are the signs and symptoms of peri-implantitis?
Following are the signs and symptoms of peri-implantitis –
- The gum tissue around the implants becomes red, swollen, and painful due to inflammation.
- Gumline receding. The “pocket” of gum in which the implant is inserted expands and deepens.
- The implant threads are exposed or visible.
- The implant is loose and moving in its socket.
- Pus is leaking from the gums surrounding the implant. Rather than something visible, it could be an awful flavor.
- Bone degradation usually is painless, but it can be observed. Jaw discomfort is a common symptom.
- When the gums become infected, bleeding ensues. There are no circumstances in which bleeding gums are healthy or normal.
- There are palpable lymph nodes in the neck or armpit that are swollen or painful.
What Causes Peri Implantitis in the First Place?
The following are the leading causes of peri-implantitis:
Immunocompromised Patients: People who suffer from an illness that affects the entire body are more likely to develop peri-implantitis. Consult your dentist about dental implants if you have diabetes or another systemic ailment. Patients may also be at a higher risk if they have ever experienced a different type of mouth infection related to peri-implantitis. If you’ve ever had periodontitis, significant gum disease, or any other bacterial mouth infection, tell your dentist.
Inadequate Oral Care: Bacteria and food particles that progressively build around dental implants and gum lines cause peri-implantitis. Diligent and consistent dental care is necessary to limit and eliminate hazardous germs found in plaque and tartar. Peri-implantitis, like most other dental disorders, can be exacerbated by smoking, drinking, or using drugs. For additional information on how to establish healthy dental practices, speak with your Periodontist.
Parafunctional Habits are unintentional habits that you may have. They can be caused by a nervous habit or a deformity of a section of your body. They can even happen while you’re sleeping. Habits such as teeth grinding, nail-biting can lead to improper tooth alignment and compromise the healing of dental implants.
Other factors that would cause peri-implantitis are –
The state of the tissue around the implant, implant design, degree of roughness of the implant surface, external morphology, and increased mechanical strain all influence the etiology of implant disease.
How to treat peri implantitis?
The prevention of bacterial infections is our top priority at Advanced Dental Implant and TMJ Center. However, when patients come to us with severe instances, our long-term goal is to arrest bone loss and retain their implants in place. Antibiotics are frequently suggested to eliminate the dangerous residual bacteria within your gums and bone, in addition to thorough cleaning of the diseased region with the correct dental instruments. Antibiotics can be delivered straight to the implant surface, if necessary.
In the most severe cases of peri-implantitis, the implant must be removed and the damaged bone replaced with bone grafts. Your dentist should open up your gums to clean the infection from the gums.
Your Periodontist should ensure that the infection has been completely eradicated before a fresh bone is grafted onto the implant. This usually entails taking a lot of antibiotics. The type of bone utilized and its physiology are essential, but there are no guarantees that the procedure will be successful.
Several factors determine a grafting’s success or failure. Having a team of dental experts on your side, who are industry leaders in sophisticated procedures, techniques, and approaches, can significantly boost your chances of success.
How to avoid peri implantitis?
People who have had gum inflammation in the past are more likely to develop peri-implantitis. However, there are several strategies to avoid peri-implantitis, including basic oral hygiene and proper dental implant aftercare.
Peri-implantitis most usually develops during the healing period following the placement of dental implants, when the location is most vulnerable to bacteria buildup.
- Observance of dental implant aftercare guidelines
- Brush your teeth twice a day.
- Floss at least once a day, ideally before going to bed
- Avoid smoking, especially throughout the healing period.
Looking for the Best Peri Implantitis Treatment?
Dr. Adatrow can help!
If you have any further questions about oral health, you can schedule a consultation with Dr. Adatrow. Dr. Adatrow has more than 18 years of experience in placing dental implants, with a success rate of over 97%, and can provide you with the best possible dental treatment. He is a Board-Certified Prosthodontist and Periodontist. Please contact our office to schedule your consultation now!
About Advanced Dental Implant and TMJ Center
Advanced Dental Implant and TMJ Center provides personalized and specialized dental treatment for patients in Desoto County, MS and Memphis, TN areas. Dr. Pradeep Adatrow is Specialist in Dental Implants and Gum Diseases and provides patients with customized treatment plans to meet the oral health needs of his patients. Dr. Adatrow is the only practicing board-certified Periodontist and Prosthodontist in the South East United States. He earned his Doctor of Dental Surgery and Post Graduate Prosthodontic Training from the University of Tennessee College of Dentistry and his Post Graduate Training in Periodontics from Indiana University. Dr. Adatrow is board certified by the American Board of Periodontology and is a Fellow of the prestigious International College of Dentistry. Along with a devoted team of dental hygienists, assistants, and administrative staff, we strive for excellence in customer satisfaction. Please visit our website at www.advanceddentaltmj.com or call us at (662) 655-4868 to schedule a consultation.



